
Choosing to remove a tooth can feel overwhelming, but extractions are sometimes the most responsible step for protecting your long-term oral health. Our priority is to preserve natural teeth whenever possible, yet there are occasions when removing a problematic tooth prevents pain, infection, or damage to neighboring teeth and tissues.
We approach every extraction with careful planning and clear communication so patients know what to expect from start to finish. Your medical history, current medications, and goals for future dental care all shape the treatment plan. That thoughtful preparation helps reduce anxiety and supports a smoother experience.
At the office of Park Dental Wellness, each procedure is performed with attention to comfort and safety. We combine modern diagnostic tools and proven techniques to make the process efficient and predictable, and to set the stage for the best possible healing and restorative options afterward.
An over-retained primary (baby) tooth that interrupts normal development
Sometimes a primary tooth does not fall out on schedule because its roots fail to resorb or because it becomes fused to the jawbone. When that happens, the permanent tooth below can be blocked from erupting properly, which can cause alignment complications. Removing the retained baby tooth at the right time can facilitate normal development and prevent more extensive orthodontic work later.
A permanent tooth with decay too extensive to restore
Dental decay is progressive: left untreated, it can destroy tooth structure, reach the nerve, and lead to abscess or spread of infection. When a tooth no longer has enough healthy structure to hold a restoration, extraction becomes the safest option to stop infection and protect your overall health.
Severe fractures or cracks that compromise the tooth
Not all chips or cracks are the same. Some can be repaired with a crown or bonding, whereas others extend deep into the root or split the tooth in a way that cannot be reliably restored. In those situations, extraction may be the most predictable way to relieve pain and prevent ongoing problems.
Advanced periodontal (gum) disease that weakens tooth support
Gum disease attacks the tissues and bone that hold teeth in place. When periodontal destruction becomes severe, teeth may loosen and become unsalvageable. Removing teeth that no longer have firm support can help eliminate sources of infection and allow for targeted treatment of the surrounding gums and bone.
Impacted or problematic wisdom teeth
Third molars often arrive late and sometimes without room to emerge properly. Impacted wisdom teeth can damage adjacent teeth, create pockets that harbor bacteria, or become a recurring source of pain. Early evaluation and, when appropriate, removal can prevent future complications.
Teeth removed to create space for orthodontic alignment
In some orthodontic cases, selective tooth removal helps achieve ideal alignment and a balanced bite. When teeth are too crowded or when jaw size and tooth size are mismatched, extractions may be part of a careful, individualized orthodontic plan to produce stable, long-lasting results.
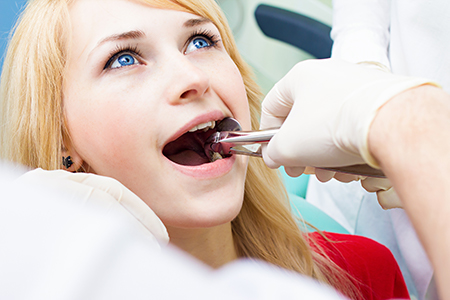
The process begins with a thorough evaluation: a review of your health history, a clinical exam, and any necessary digital radiographs to understand root anatomy and the relationship to surrounding structures. This information guides whether a tooth can be removed in a straightforward manner or whether a more involved surgical approach will be needed.
We discuss anesthesia and comfort options so you can choose the level of sedation that suits your needs—ranging from local anesthetic alone to additional calming measures for more anxious patients. We also address medical considerations, such as current medications or systemic conditions, that could influence preoperative planning or require coordination with your physician.
Before the procedure, the treatment steps and recovery expectations are reviewed in plain language. Our goal is to remove the tooth with the least disruption to the surrounding tissues and to present restorative or replacement options afterward so you can make informed decisions about your smile’s future.
A simple extraction is performed on a tooth that is visible in the mouth and has a predictable root shape. After numbing the area, the dentist gently loosens the periodontal ligaments and employs specialized instruments to deliver the tooth with care. The emphasis is on minimizing trauma to the gum and bone while ensuring complete removal.
Patients often appreciate the straightforward nature of this procedure and the relatively quick recovery that follows. We provide detailed aftercare instructions and are available to manage discomfort or questions during healing to help you feel supported every step of the way.
Surgical extractions are used for teeth that are broken at the gum line, fused to bone, or impacted beneath the surface. This approach may require a small incision in the gum and the selective removal of a bit of bone to access and extract the tooth safely. Such cases sometimes require referral to or collaboration with an oral surgeon when specialized surgical care is indicated.
Even in surgical cases, anesthesia and comfort are closely managed, and alternatives for sedation are discussed ahead of time. Postoperative planning focuses on infection control, comfortable healing, and timely follow-up to monitor recovery.
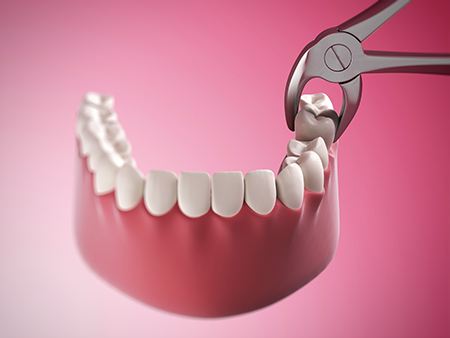
Recovery after an extraction typically follows a predictable course: initial bleeding and swelling, followed by gradual reduction of discomfort and tissue healing over days to weeks. Most patients can manage their recovery at home by following simple, evidence-based instructions that protect the healing clot and reduce the chance of complications.
We give personalized guidance based on the complexity of your extraction and your overall health. This may include temporary activity limits, medication recommendations, and when to return for a follow-up appointment. Clear instructions and prompt communication help ensure a smooth recovery.
If concerns arise—such as excessive bleeding, increasing pain, or signs of infection—we ask that patients contact the office so we can assess and respond quickly. Early attention to problems is the best way to avoid delays in healing.
Maintaining pressure with gauze
Your clinician will place gauze over the extraction site and ask you to bite down to form a stable clot. Replace gauze as directed and maintain firm, steady pressure during the first hour or until bleeding slows. A small amount of oozing for 24 hours is common; persistent heavy bleeding should be reported to the office.
Protect numb tissues
Until the anesthetic wears off, be careful not to chew or press your lips, cheeks, or tongue near the numb area to avoid accidental injuries.
Take medications as directed
If antibiotics are prescribed, take the full course as instructed. For pain control, use recommended over-the-counter or prescription medications according to directions and contact the office if pain is not manageable with the prescribed approach.
Protect the blood clot
Avoid rinsing vigorously, spitting forcefully, or using straws for the first day or two. These actions can dislodge the clot and impair healing. Let any mouth rinses fall gently from your lips into the sink rather than spitting.
Control swelling with ice
Apply an ice pack to the cheek in short intervals during the first 24 hours to minimize swelling. After the first day, warm compresses may help if stiffness persists.
Avoid tobacco
Smoking and tobacco products impair clot formation and slow healing. Avoid all tobacco for at least a week after the extraction to reduce the risk of complications.
Choose gentle foods
Stick to a soft, nourishing diet at first and avoid very hot, spicy, or carbonated beverages until comfort improves. Hydration is important, so sip water frequently.
Maintain careful oral hygiene
Continue brushing gently, avoiding direct trauma to the extraction site. After the initial 24–48 hours, a mild warm saltwater rinse can help keep the area clean; follow the timing and technique we provide.
Keep follow-up appointments
If sutures were placed or if a complex extraction was performed, keep your scheduled follow-up so we can confirm proper healing and address any concerns.
If you experience unusual symptoms—such as worsening pain, prolonged bleeding, or fever—please contact our office for guidance so problems can be addressed promptly.
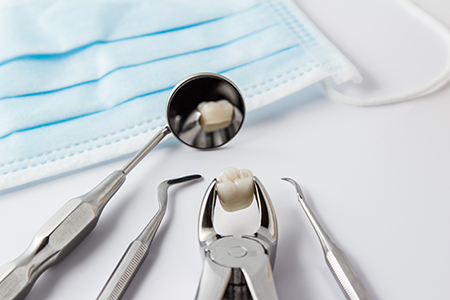
Extracting a tooth is a restorative decision made to protect your wider oral health, and it should be performed with clinical skill and compassion. Our team emphasizes clear communication, careful technique, and individualized aftercare so that each patient feels informed and supported throughout the process.
We also discuss tooth replacement options—such as removable prostheses, fixed bridges, and dental implants—when appropriate, and we help patients plan the sequence of treatment that best fits their overall goals for function and appearance. Your long-term oral health guides every recommendation we make.
In short, our approach is to balance conservative care with proactive solutions, prioritizing predictable outcomes and patient comfort at every stage.
Summary: Tooth extractions can resolve pain, remove infection, and protect adjacent teeth when preservation is no longer possible. Careful evaluation, a clear treatment plan, and sensible aftercare make the experience as smooth as possible. Contact us for more information about extractions or to discuss your individual treatment options.

Tooth extraction is recommended when a tooth cannot be preserved with predictable restorative or periodontal treatment and is causing or risking harm to surrounding tissues. Common clinical indications include extensive decay that destroys supporting structure, severe fractures that extend below the gum line, advanced periodontal disease with loss of support, and teeth that are impacted or causing recurrent infection. The decision to extract is based on a comprehensive evaluation of radiographs, clinical findings, medical history, and the patient’s long-term oral health goals.
At our office the focus is always preservation when feasible, but extraction becomes the healthiest option when it prevents spread of infection, alleviates pain, or protects adjacent teeth and bone. Treatment planning also includes discussion of replacement options and the sequence of care so patients understand how extraction fits into their overall oral health plan. Clear communication about risks, benefits, and expected outcomes helps patients make informed decisions that align with their needs.
A simple extraction is performed on a fully erupted tooth that is visible in the mouth and has a predictable root form; it is typically completed with local anesthesia by gently loosening the periodontal ligaments and removing the tooth with elevators and forceps. These procedures are often shorter, involve less tissue manipulation, and generally have a quicker recovery when compared with more complex cases. Simple extractions are appropriate when the tooth structure and surrounding bone allow easy access and removal.
Surgical extraction is used when a tooth is broken at the gum line, impacted, fused to bone, or otherwise not amenable to straightforward removal. The clinician may need to make a small incision, remove a bit of bone, or section the tooth to extract it safely, and this approach sometimes requires collaboration with an oral surgeon. Surgical cases usually require more detailed preoperative planning and postoperative monitoring to ensure proper healing.
Preparation starts with a thorough medical and dental history review, current medications, and any necessary radiographs to evaluate root anatomy and proximity to important structures such as nerves or sinuses. Inform your clinician about blood-thinning medications, recent illnesses, pregnancy, heart conditions, or any systemic issues that could influence anesthesia or healing so the team can coordinate care with your physician if needed. Follow any preoperative instructions provided, such as fasting guidelines for cases requiring sedation and stopping or adjusting medications only when directed by your prescribing clinician.
Arrange for transportation if you will receive sedation beyond local anesthesia, and plan for a period of limited activity following the procedure to promote healing. Wear comfortable clothing and avoid alcohol or tobacco before your appointment, as these substances can affect anesthesia and clotting. Bringing a list of questions or concerns to the consultation helps ensure you understand the procedure, expected recovery, and next steps for tooth replacement if applicable.
Anesthesia options range from local anesthesia that numbs only the treatment area to oral or intravenous sedation and, in select cases, general anesthesia for more complex surgical procedures. Local anesthesia is routinely used and has an excellent safety profile; sedation can be added for patient comfort and anxiety management, with dosing tailored to medical history and the complexity of the extraction. All anesthesia and sedation choices are discussed ahead of time, and monitoring protocols are in place to maintain safety throughout the procedure.
Prior to sedation, your clinician will review your medical history and current medications to identify any risks or necessary modifications, and appropriate monitoring equipment is used during treatment. If you have significant medical conditions, the team may coordinate with your physician to determine the safest approach. Clear preoperative instructions, adherence to fasting guidelines when applicable, and post-sedation recovery protocols contribute to safe, comfortable care.
Wisdom teeth commonly cause issues because they erupt late and there may not be adequate space for them to emerge properly, which can lead to impaction, damage to adjacent teeth, cyst formation, or recurrent infections. These third molars should be evaluated with clinical examination and radiographs during adolescence and early adulthood so the clinician can monitor development and anticipate potential problems. Early assessment allows for informed decisions about observation versus extraction before symptoms or complications arise.
Removal is often recommended when wisdom teeth are partially erupted with a high risk of infection, are impacted in a position that threatens neighboring teeth, or create pockets that are difficult to keep clean. The timing and complexity of removal depend on root development and the tooth’s relationship to adjacent anatomical structures, and recommendations are individualized to balance risk and long-term oral health benefits.
Yes. Extractions are sometimes integrated into orthodontic treatment to address severe crowding, tooth-size and jaw-size discrepancies, or to improve bite relationships and facial balance. When space is limited, removing one or more teeth can create the room needed to align teeth predictably and establish a stable, functional occlusion. Orthodontic treatment planning involves collaboration between the orthodontist and restorative dentist to determine which teeth, if any, are appropriate to remove for optimal long-term results.
The decision to extract for orthodontic reasons is individualized and takes into account age, facial esthetics, airway considerations, and the overall treatment objectives. When extractions are recommended, the sequence of care is coordinated so that surgical and orthodontic phases proceed smoothly, and restorative options after alignment are discussed to ensure a durable and functional outcome.
While most extractions heal without incident, possible complications include prolonged bleeding, infection, delayed healing, and a painful condition known as dry socket where the blood clot is dislodged from the socket. Nerve injury is a rare but important risk with extractions near the lower jaw’s sensory nerves, and sinus communication can occur with upper molar removals in close proximity to the sinus floor. Thorough preoperative assessment and careful technique reduce these risks, and patients are informed about signs to watch for after the procedure.
Prompt communication with your dental team is essential if you experience increasing pain, fever, persistent or heavy bleeding, numbness that does not resolve, or any other concerning symptoms. Early assessment and appropriate interventions—such as medication, socket care, or referral—help resolve complications quickly and minimize long-term effects. Following postoperative instructions and attending follow-up visits supports predictable healing.
Initial care focuses on protecting the blood clot, controlling bleeding, minimizing swelling, and preventing infection. Bite gently on gauze as instructed to maintain pressure, avoid rinsing or spitting vigorously during the first 24 hours, and refrain from using straws or smoking because suction can dislodge the clot and increase the risk of dry socket. Use ice intermittently during the first 24 hours to limit swelling and rest with your head elevated to reduce bleeding and discomfort.
Take medications exactly as prescribed, complete any antibiotic course if indicated, and consume soft, cool or lukewarm foods that do not irritate the area. After 24 to 48 hours, begin gentle saltwater rinses as recommended to keep the site clean, and continue to avoid poking or probing the socket with fingers or tongue. If sutures were placed, follow the timeline given for suture care and return for scheduled follow-up so healing can be evaluated.
Most patients see the most significant pain and swelling within the first 48 to 72 hours, with steady improvement thereafter as soft tissues begin to close and inflammation subsides. Initial tissue repair occurs over the first one to two weeks, while deeper bone remodeling and full maturation of the socket can take several months. Recovery speed varies by extraction complexity, patient health, age, and adherence to postoperative instructions.
Simple extractions commonly allow return to normal daily activities within a few days, whereas surgical or more involved cases may require a longer period of limited activity and additional follow-up care. Your clinician will provide specific expectations based on the procedure performed and will schedule a follow-up to confirm healing or to guide the next phase of restorative treatment if needed.
After extraction, several replacement options exist to restore function and appearance, including removable partial prostheses, fixed dental bridges, and dental implants. Each option has specific clinical requirements and benefits: removable prostheses provide a noninvasive interim or permanent solution, bridges restore adjacent tooth contacts when suitable abutments exist, and implants replace the tooth root to support a stable, natural-feeling crown. The choice of replacement depends on bone availability, adjacent tooth condition, overall oral health, and the patient’s long-term goals.
Planning for replacement often begins before or shortly after extraction to preserve bone and optimize outcomes; ridge preservation techniques or timely implant placement can influence future prosthetic options. Discussing these choices with your dental team allows creation of a coordinated treatment plan that addresses both immediate healing and the desired restorative result. Park Dental Wellness can help evaluate the options and sequence treatment to meet your functional and esthetic objectives.
Contact the office promptly if you experience uncontrolled bleeding, a fever or signs of systemic illness, severe or worsening pain that is not relieved by prescribed medications, persistent swelling beyond the expected timeframe, or numbness that does not resolve. Additionally, contact the team if you notice unusual drainage from the site, a foul taste that suggests infection, or if sutures become loose or dislodged prematurely. Early communication enables timely assessment and appropriate intervention to prevent more serious complications.
Routine postoperative questions are also appropriate to bring to the office, such as concerns about diet, medication interactions, or care of the extraction site. Your dental team is available to clarify instructions, arrange follow-up visits, and provide reassurance during healing so you can recover comfortably and confidently. If you are uncertain whether symptoms require urgent attention, it is best to call and have your situation evaluated.

At Park Dental Wellness, reaching us is simple. Whether you have questions about treatments or are ready to schedule your next visit, our friendly team is here to guide you every step of the way. Call, email, or use our convenient online form—we’ll make sure your experience is easy, comfortable, and tailored to your needs.
Start your journey to a healthier, more confident smile today!